If you’ve recently lost a child, there’s something I want you to know. Because I’ve been there too.
At the end of 2017, I found out I was pregnant. We were shocked. We weren’t actively trying, so when it happened, I hardly knew how to process it. I was extremely sick and could barely eat.
A few weeks later, we were even more shocked to find out I was pregnant with TRIPLETS. We always thought it would be fun to have twins, but to be blessed with triplets was an even bigger gift that we were so thankful for.
But when I began researching “pregnancy with triplets”, I started to get nervous. It was considered high-risk—there could be so many complications—they would definitely be born premature and I’d need to have a C-section. These were all things I’d never experienced before.
The challenges started with finding a doctor. I was turned down by five different doctors, because nobody wanted to deal with the high-risk challenges of a triplet pregnancy.
I was an emotional mess. But after a lot of research, I finally found a team of high-risk doctors at our local university hospital.
They’re all girls!
My first few visits went okay. I found out the babies were identical and all shared a placenta. I also found out that Baby A had marginal cord insertion (MCI), which means her umbilical cord wasn’t attached to the center of the placenta (where all the nutrients come from).
Of course, I went to Dr. Google to research this, and found out that MCI is usually okay, but there’s a possibility that the baby could stop growing or have cord issues that prevent blood flow and oxygen to the baby. So, naturally, I was terrified.
But I was excited to be able to find out whether the babies were boys or girls. Since they were identical, they were the same sex. We found out that we were having three little girls, and we couldn’t be more excited for their arrival.
I also recorded their heartbeats and put the recording inside stuffed lambs as a keepsake. We announced it to our other kids and recorded that too — we were all so excited, especially my oldest daughter!
And aside from extreme nausea, heartburn, occasional dizziness and no appetite, my pregnancy was pretty uneventful. My biggest concern was having healthy babies.
Once I found out the babies were all girls, it was ON! All. Pink. Everything.
I went shopping like a mad woman. I knew my babies would be premature and I also found out that I may be put on bedrest towards the end of my pregnancy, so I really wanted to be prepared early.
I loved choosing all of their names: Bella Marie, Bailey Marie and Brooklyn Marie—Marie is a family name on their dad’s side. Bella was our Baby A, the one with the MCI, and the sonographer and doctor kept a close eye on her.
Goal: 28 weeks
At 22 weeks, I found out that Bella was growing a lot slower than Bailey and Brooklyn. So I started getting ultrasounds every week, and Bella grew very little over the next few weeks. They diagnosed her with IUGR (intrauterine growth restriction), and at 25 weeks, I was informed that she had abnormal (elevated) cord flow.
We agreed that I would go on hospital bedrest starting at 28 weeks, because things could take a turn very quickly. One of the biggest and scariest risks of having identical multiples is that sometimes in the womb they begin to steal nutrients from each other, preventing proper growth — this is called twin-to-twin-transfusion syndrome, or TTTS.
If we made it to 28 weeks, the babies would still be very premature, but as each week went by and they continued to stay inside, they had a better chance for survival.
At 28 weeks, I was admitted to the hospital for bedrest and monitoring, and the next 5 days were a blur. I got an ultrasound once a day, and fetal NST(non-stress test) to check the babies’ heartbeats twice a day. I was also given meds for nausea, heartburn and insomnia, and I received iron supplements through IV along with daily fluids.
It was difficult, to say the least. I missed my kids at home and I missed my bed, and I was scared for my babies.
Call your husband now
On June 5th, I received my breakfast when the nurses came in to strap me up for the NST. The babies were moving all over the place. They finally got me strapped up, but after about 30 minutes, they were back. They unhooked me and told me I’d be going down to labor and delivery for monitoring.
What?! Why?? I thought. I was scared out of my mind. I kept thinking: I’m not ready! I’m only 28 weeks and 5 days! It’s too soon!
Once I was in L&D, the nurse calmed me down and told me it was only for monitoring. I saw a warming bed for a newborn and freaked out that this was all happening so quickly. I hardly had time to process everything.
Then, they couldn’t locate the babies’ heartbeats and they were moving a lot, so my sonographer came to try and help locate them.
My MFM team also came to do some scans. During the scan, they noticed that Bella’s cord flow was absent and she was getting zero oxygen from her umbilical cord. My MFM informed me that we’d more than likely be delivering very soon—like within the next few days or so.
I was totally overwhelmed by all of this. Everyone left the room and it was just me and the babies and their little heartbeats that I could hear through the monitor. Daddy went to run a few quick errands, and I fell asleep.
But then, all of a sudden, the MFM team rushed in. He looked directly at Bella’s machine and said, “Call your husband now. We’re about to deliver.” I texted him, “Come now!” And he was there in 5 minutes.
I had never seen babies so small
As they prepared me for delivery, I was more nervous than I’ve ever been about anything in my life. I have always feared a C-section, and it was just too early! I received a magnesium drip to help with the babies brains and it made me feel like I was on fire.
Once in the operating room, Daddy got dressed in surgical gear and it was game time! The next 30 minutes happened so fast, but at the same time, in slow motion. I remember when each baby came out and my hubby properly identified each baby’s placement. I remember looking to my left and seeing Bella in the bed before they whisked her off to the NICU.
They put Brooklyn right next to my face. We locked eyes, and I said, “Hey Brooke” before they took her away. I didn’t see Bailey until later that night.
The babies were all extremely small. Because they were born so early, they were considered micro-preemies, and they were all tiny.
Bella weighed 1 pound, 4oz.
Bailey weighed 1 pound, 14oz.
Brooklyn weighed exactly 2 pounds.
I went to the NICU a few hours later to see them and I felt like an emotional mess. I’d never seen babies so small. They were all under the jaundice lights and hooked up to so many wires, cords and tubes. Brooklyn was on a ventilator because she had the most trouble breathing.
But Bella and Bailey were both on CPAP and basically breathing on their own! Bella was doing wonderfully! The nurses all said it seemed like she was a case of better out than in.
I knew it would be awhile before we could hold them. They had lines going through their umbilical stump so that the doctors could draw blood and quickly fuse meds or fluids if needed — they couldn’t quite place regular PICC lines (baby IVs) in their arms yet, and we had to wait on that before we could hold them.
We visited with the babies for a while and then I went back to the postpartum recovery room empty-handed. I knew I had just given birth to three babies, but I felt so empty.
Waiting to hold my babies
The next few days were really tough. I almost passed out in front of the NICU. They took my blood pressure, and it was high, so the hospital decided to keep me for an additional 2 days.
I was also diagnosed with postpartum anxiety, and my husband had to go out of town for work. He put a relative in charge of visiting me and caring for me but due to personal issues, I told them not to come. I was miserable and lonely.
When I was finally discharged, leaving my teeny tiny babies at the hospital was one of the hardest things I’ve ever done. But surprisingly, once I got home, I actually felt better—relieved to be in my own home again.
Over the next few days, I pumped milk constantly and called and/or visited the NICU every day. I would sit with my babies for hours at a time. I cried every time I saw them.
On Wednesday, June 13th, Bailey and Brooklyn got their PICC lines and I was finally able to hold them! They were 8 days old. But Bella didn’t have hers yet. They had attempted, but it wasn’t successful, so they wanted to wait another day or so before trying again.
After running back and forth to the NICU for so many days in a row while still recovering from my C-section, my body was tired. I didn’t visit the NICU on Thursday, the day Bella got her PICC line. But I knew I’d be able to hold her the next day and I couldn’t wait.
Overnight, my world shattered
On Friday, June 15th, I called the NICU to check on the girls as usual. “Bella got her PICC line last night, so I can hold her now, right?” I asked. But the nurse said, “Well, we’re going to have to hold on that for now because she’s now showing signs of infection. We’re going to stop her feedings and start her on antibiotics.”
Those words hit me. Hard. Infection? How? Why? What happened??
The nurse then started a laundry list of things going on with my baby.
She had gone from breathing on her own to being intubated and needing assistance breathing. She was on 50% oxygen. Her PH levels were high. Her blood pressure was low, so she needed blood pressure meds. Her heart rate was low. She was anemic, so she needed iron. Her blood count was low, so she needed a blood transfusion. Her PDA valve was open. And they also detected a slight heart murmur.
I could barely process what the nurse was saying as my world shattered. What had happened in a day? How did she get an infection? Is it my milk? They assured me it wasn’t my milk—all the girls would be sick if it was.
I had so carefully worn gloves when I visited. I scrubbed down every time. I wore a gown.
How did my baby get an infection? Are y’all going to fix it?? My thoughts went in circles and I felt horrible. I should’ve come yesterday. It’s my fault for not coming. I could’ve caught on to her giving signs. I would’ve known. Mom guilt on 100.
The rest of that day and the next day, I was in and out of the NICU visiting the girls, but paying extra attention to my little Bella.
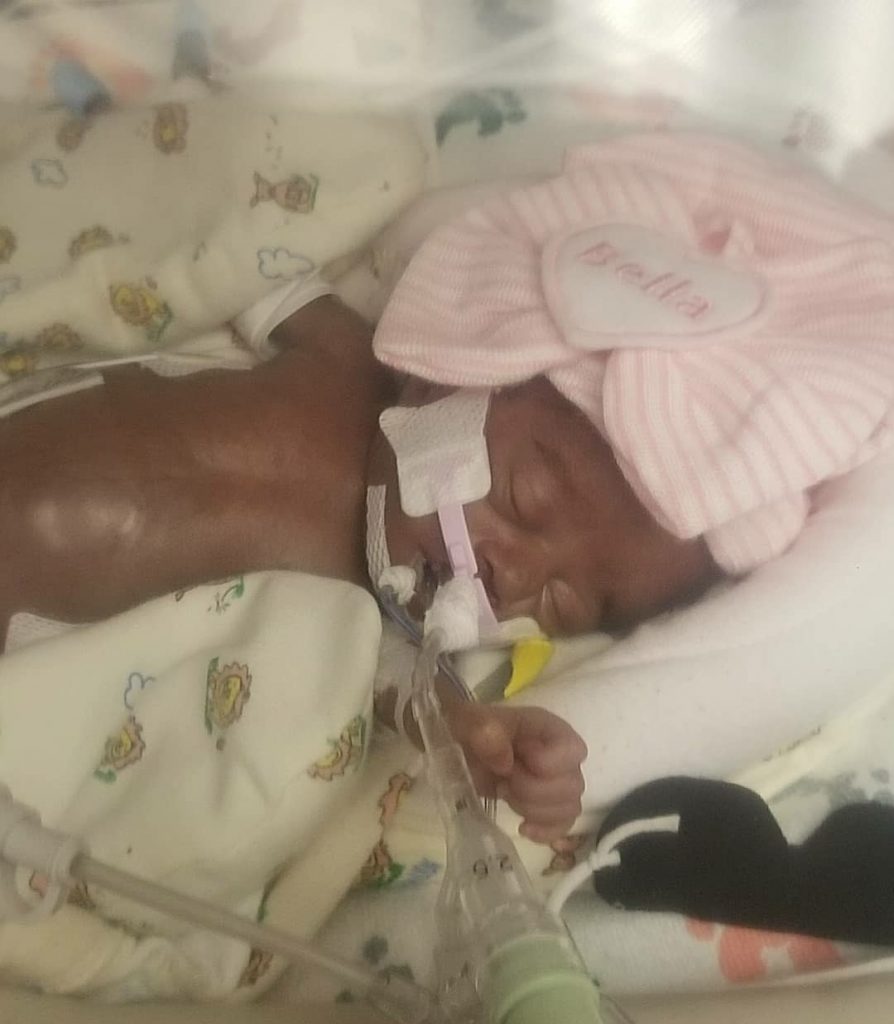
I begged her to keep fighting
On Saturday, June 16th,right before midnight, we walked into the NICU and Bella was under the ultraviolet lights. Her bilirubin levels had shot up. She was also on antibiotics, lipids, blood pressure meds, caffeine and a slew of other things.
The doctors had been at her bedside all night. They were running tests, drawing labs every hour and still trying to figure out what exactly was wrong with her. They knew it was an infection, but didn’t quite know which one.
The doctor told me, “We’re trying to keep your baby alive long enough for the antibiotics to kick in.” I shook my head. No! That’s not how this is supposed to go! How did my baby get an infection? She was fine! She was perfect! Now she’s all of a sudden facing death? No! How??
I reached in to touch her and they turned the lights off and removed the eye protector. My baby was pale. I talked to her. I cried. I prayed. I begged her to fight, to keep fighting.
Even though I knew she was in pain, I couldn’t lose her. I delivered three babies dammit! How could I lose one? As they started preparing for more labs, I told them I was going home to get some rest and I’d be back first thing in the morning, with instructions to call me immediately if ANYTHING changed.
An hour later, we were in the car headed home. The ride was quiet. Long. I realized it was Father’s Day — Sunday, June 17th. I prayed in my head, begging God please, please not to take my baby from me. What did I do to deserve this?
My husband tried to reassure me that it was part of the process of NICU —babies get sick, but that’s why they have a good team of doctors. God wouldn’t give us this amazing blessing just to take it away.
But his words were empty to me. I knew what I had seen, and heard what those doctors said to me. I was scared out of my mind.
Praying for a miracle
Once we got home, I put on some Gospel music and I prayed. And I prayed. And I prayed. I begged and pleaded with God. I cried. I closed my eyes for a few seconds and I felt my phone buzz. The words “NICU” made my heart sink.
The doctor said, “Bella is now on 100% oxygen and all of her levels have either maxed or bottomed out. We’re doing all we can.” Through my exhaustion and headache from crying and worry, I somehow told her we were on the way.
I just remember screaming Cedric’s name and telling him, “Let’s go.” We flew down the highway, parked illegally, and rushed to the NICU.
When I saw my baby, I told them, “Put her hat on her, she’s gonna get cold.”
Her heart rate was barely over 100 (it should’ve been between 140-160). Her oxygen was in the low 40’s (it should’ve been above 85). Her numbers were slowly decreasing, but every time I talked to her, they raised ever so slightly. That gave me hope.
But it wasn’t enough.
At 1:57 am the doctor said to me, “Would you like to call your pastor or family members to come pray or see her? We don’t see her making it through the next 24 hours.”
I almost screamed at her. “NO! I speak life into my baby. Don’t you dare write her off or try to seal her fate. She’s responding to my voice! She’s getting better.”
I talked to my baby like I did when she was in my belly. I carried her for 28 weeks and 5 days. We had a bond. And Bella was my favorite name.
I kept thinking, She can’t leave me. Her siblings have never met her. She can’t leave them. Babies aren’t supposed to die. It’s not the natural order of things. My children should bury me!
As I talked Bella, I started recording our time together. I wanted all the memories I could get.
The doctor also suggested that I hold her, as her numbers began dropping rapidly.
I don’t go to church, so I didn’t have a pastor to call on. Cedric tried calling the pastor that he grew up with, but he didn’t answer. I called my sister and asked her to come see Bella.
As they were preparing her so I could hold her, I was still recording. I was still talking. I was still crying. This was like a bad dream. They placed my baby in my arms for the first time. My baby was 12 days old, dying, and this was my first time holding her. I lost it.
I told her she did a good job fighting. She did what she could do. I told her I know she’s tired and it’ll be selfish of me to ask her to keep fighting. I just didn’t want to lose my baby. I told her if she’s tired of fighting, to let go. Mommy will be ok. She was so strong. So, so strong.
My last words to her were, “I love you and I’m gonna miss you”. Then they unplugged her. My baby was gone.
The worst pain I could ever imagine
At that moment, I didn’t care about the other families in the NICU. I didn’t care about the other babies. I lost my child and it hurt like hell! I cried so hard, my C-section incision burst open. That pain was nothing compared to losing my baby. I was numb.
My phone was still recording and it captured our final moments together.
All the memories I have of my baby are in my belly and in the NICU where she passed. The only pictures I have are ultrasounds and in the NICU where she passed. I hated the place.
I kept thinking: How is this my reality? What did I do to deserve such pain? I’ll never get over this.
For a brief second, I forgot we had two other babies there. I was scared to bond with them. I was afraid of losing them too.
How do you move on?
While the world moved on, my sorrow and grief washed over me. I carried the memory of my baby’s life as well as the memory of her death. How do you move on from that?
At some point over the next few days, we picked out a pink casket and planned a funeral for our baby. We buried her in the infant section of the cemetery. I told myself that I must pick myself up because I still have 2 preemie babies in the NICU.
I knew having preemie babies came with a lot of risks, but I never imagined I could lose one of my babies after they were born.
But after losing Bella, I was extremely hands-on in my survivors’ lives. And the girls did amazingly well in the days and weeks following her death. They met milestone after milestone and I was one proud mama!
So many preemie babies are so strong and resilient. My girls were three months premature, but they are doing everything they’re supposed to be doing—there are no developmental delays for their adjusted (and sometimes actual) age. Though, I often wonder if they remember Bella.

One day at a time
My story isn’t an easy one to read, or to tell. But by sharing honestly about my experience, and also by documenting my journey on social media, I have received such an outpouring of love and support from my online community that it’s been incredibly healing for me. And I’m forever grateful.
So now, when people ask me: “How do you do it? How do you go on after losing a child?”
I tell them: “One day at a time.”
I live by this. I stand by this. It’s what has gotten me through the NICU, losing Bella, being present for my survivors and other children, and moving forward as a grieving mother.
One day at a time.
In the tough moments, I remind myself to take each day as it comes. There are good days and there are bad days, and it’s okay to NOT be okay sometimes. This is part of our grief and part of our healing and it takes a lot of time to process this.
Yes, losing a child is the worst possible thing I can ever imagine happening to anyone—it feels like the end, like there is no hope, like you’ll never heal.
But there IS hope, mama. You will never, ever forget your child, no matter how many years go by — but with time, you can find peace and healing. And you are not alone.

I hope by openly sharing about my experience and my grief, I can help encourage and other moms who are navigating life after child loss. If my transparency can help just ONE person know that you’re not alone, I’ve feel like I’ve done my part.
To all of the mamas keeping endless watch at the side of a little bed in the NICU: stay strong and keep fighting for your little one. Take each day—one at a time.
And to all of the mamas who leave the hospital empty-handed and alone: the days are long, and the nights are longer, but it does get better, one day at a time.
Even after losing my baby, there was light at the end of my tunnel. And there will be light for you too.
Follow Nicole’s healing journey on Instagram: @my.triplets.journey


I love it!!! ❤️ You are the strongest woman I know. This brought back all the emotions.
Nicole, youve done it again! You just keep giving it to an and giving it to an and doing it to seamlessly. You are, and this is what the world needs more of. I watched it all under fold and I’m still watchimg amd rootimg for you. My sweet little cub is 15, but from now on every year I will remind you when “I’ start planning. “WE” will start planning. 5 June & 6 June will always OUR dates lady! 🐝 🐝 🐝
@hurricanerita
Thanks for sharing your story and your transparency Nicole. Took me back to some of both of my NICU experiences. Your definitely a strong mama who will go on to help many in their journey. Be blessed always and Happy 1st Birthday to your strong survivors! Happy Heavenly Birthday to your sweet angel Bella!
Nicole, I don’t even know you but I felt all of this. Through my years I send you prayers, one day at a time or what I often say, “One moment at a time.”